What problem are we solving?
More than half a billion people worldwide suffer from unhealthy glucose regulation, many of whom are unaware, young, and notably do not have a diagnosis of diabetes.
That’s because metabolic health is a spectrum — not just “diabetic or non-diabetic."
And we often don’t know where we fall on this spectrum until we’re at the extreme and unhealthy end of it.
“Today, a staggering 93% of the US population is considered metabolically unhealthy, and 74% are considered overweight or obese,” said Anttoni Aniebonam, CEO and Co-Founder of Veri.
“Poor metabolic health is quickly becoming one of the biggest healthcare crises in the world. With this new feature launch, we’re a couple of steps closer to solving it.”
What is metabolic healthspan?
Metabolic Healthspan is the period of your life spent in good metabolic health. This new metric reflects the impact of your diet, exercise, and lifestyle by showing you how many years you may extend this period - and the five evidence-based measures that support it.
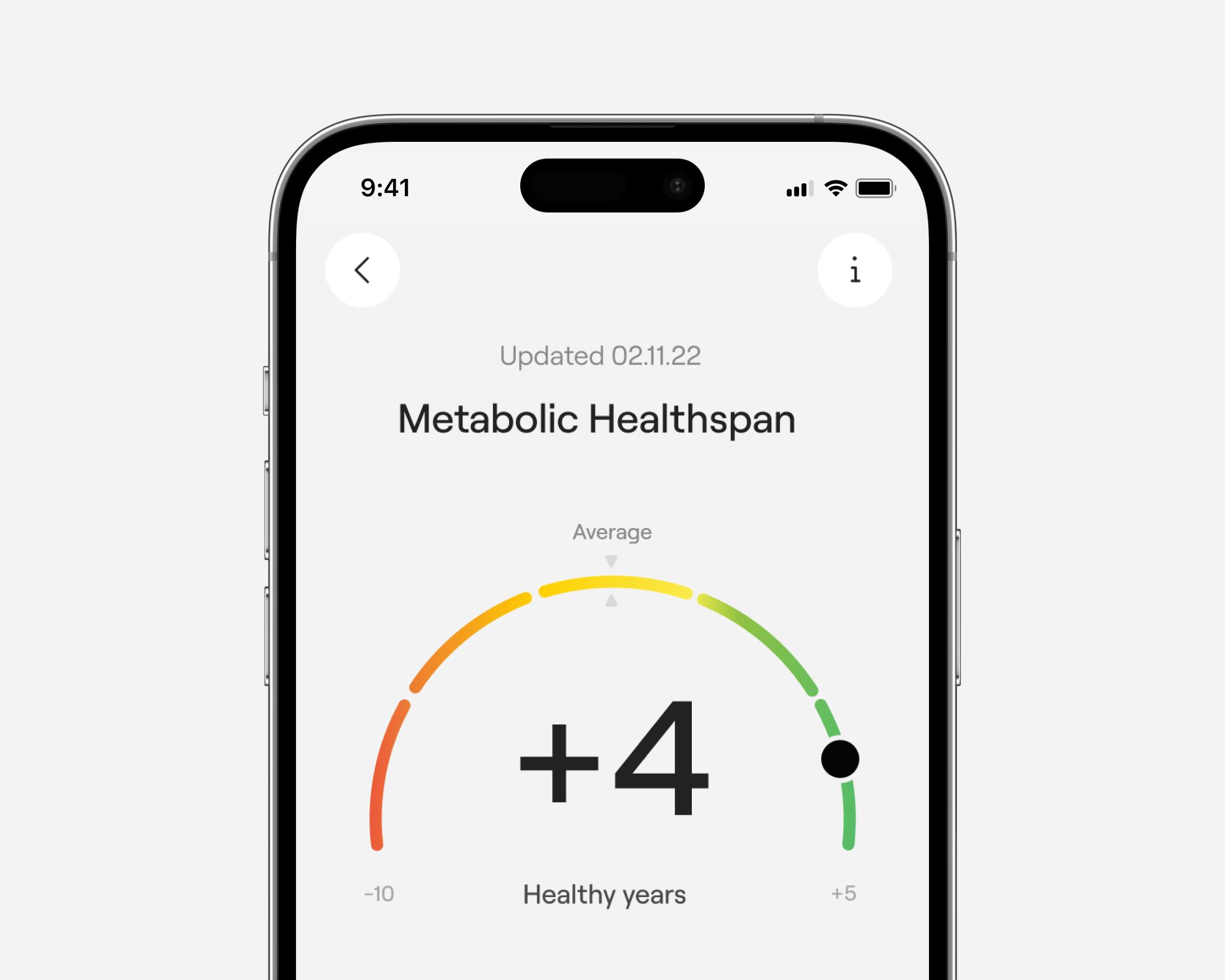
Metabolic Healthspan was co-developed with Veri’s advisors of researchers, endocrinologists, and cardiologists from universities like Stanford and Harvard and institutions such as the American Diabetes Association (ADA) and Centers for Disease Control and Prevention (CDC).
Our metric integrates 5 evidence-based metrics — average glucose, morning fasting glucose, glucose variability, glucose oscillation, and body mass index (BMI) — to give users never-before-seen insights into the state of their metabolic health and how they can improve.
It is a guiding metric for Veri’s users to understand how to improve their metabolic health over time.
With the addition of Metabolic Healthspan, Veri is closing the loop on measuring metabolic health outcomes.
As Veri Advisor and Harvard Medical School professor Dr. Fatima Cody Stanford notes, “For optimal metabolic health, we must know our metrics. A large portion of the population has glucose dysregulation. Veri empowers the user with the knowledge to know their metrics and make shifts to ensure optimal metabolic health. Each person is unique, and knowledge is power.”
Where other metabolic health apps have failed to show long-term progress, Metabolic Healthspan not only paints a holistic view but provides real insights into how to improve.
Our users care about everything from reversing insulin resistance to losing weight to maintaining their health as they age. Metabolic Healthspan gives them a clear picture of the status of their metabolic health that isn’t possible from a scale, a glucose tolerance test, or even an Hb1AC test.
How is metabolic healthspan calculated?
Metabolic health is defined by glycemic control, insulin resistance, and body weight. Poor metabolic health is a predictor of major age-related diseases, including cancer, diabetes, heart disease, and stroke. Metabolic Healthspan integrates five key science-based measures that capture glycemic control (insulin resistance) and body weight to give you a better indicator of your health.
The five contributors shown below are weighted to show how your Metabolic Healthspan may be improved.
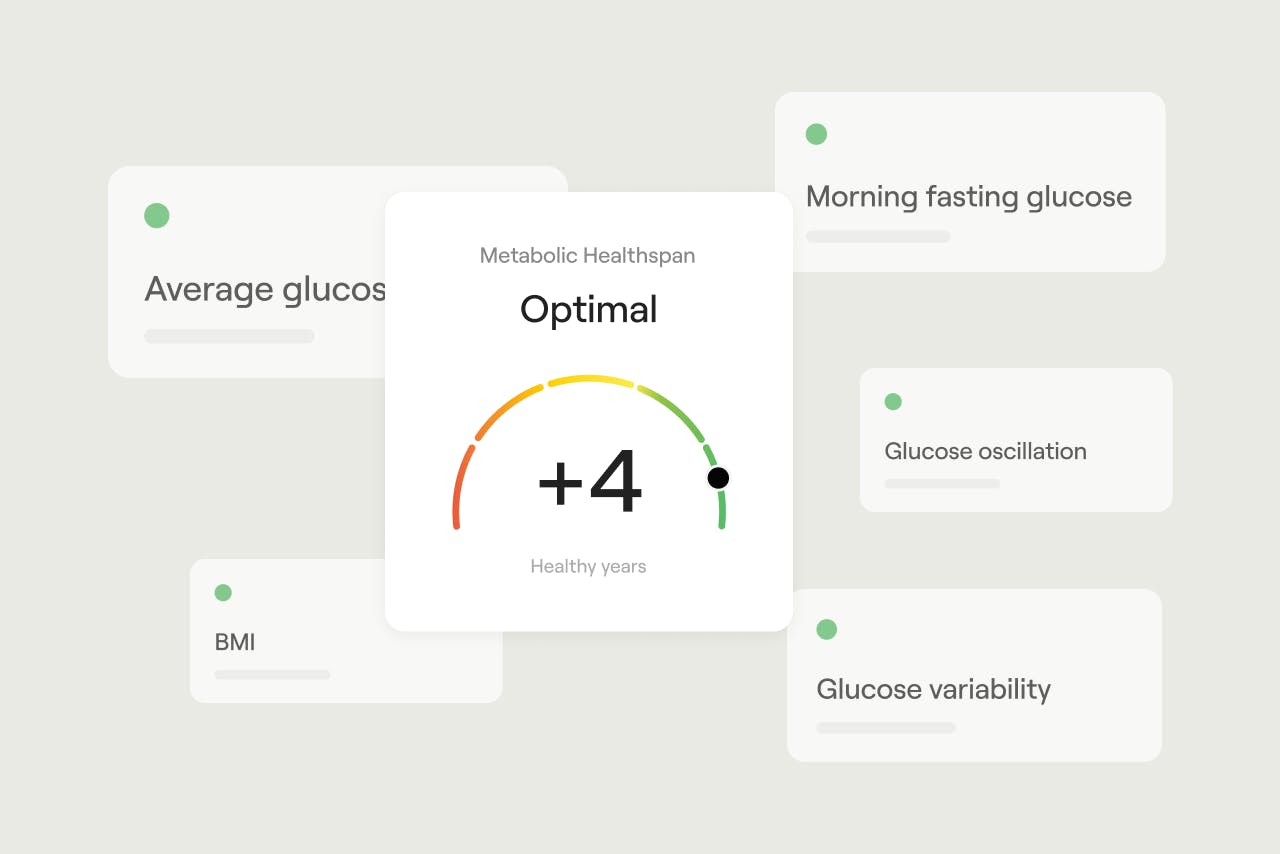
1. Average glucose
Average glucose represents the mean glucose level for a given day (24h) and is intended to give you an overall sense of your daily glucose level. Studies have shown that a larger percentage of the population unknowingly has glucose levels that are above the ideal range, often in the prediabetes or diabetes range [1, 2].
2. Morning fasting glucose
Morning fasting glucose is a robust indicator of insulin sensitivity or resistance. The American Diabetes Association (ADA) uses morning fasting glucose levels to determine whether an individual may have signs of early insulin resistance (impaired glucose tolerance) or diabetes. A morning fasting glucose level of > 99 mg/dL (>5.5 mmol/L) is one of the diagnostic criteria for pre-diabetes (or early insulin resistance) based on ADA guidelines [3].
Studies have demonstrated that your fasting glucose level is associated with a higher rate of mortality, diabetes, heart and vascular diseases, and impaired brain health [4, 5, 6].
3. Glucose variability
Glucose variability, as measured statistically by standard deviation (SD), refers to how much your glucose varies within a given day. Generally, a lower variation of glucose levels throughout the day, reflecting more stable glucose levels, is better for overall health [7, 8]. A high variation, reflecting more prominent rises and falls in your glucose throughout the day, may be detrimental to your health.
4. Glucose oscillation
The mean amplitude of glycemic excursion (MAGE) is a measure of how intense your glucose spikes and dips are in a day. It is defined as the average of readings that exceed one standard deviation of the daily mean.
MAGE is commonly used to represent glucose fluctuation or oscillation, which contributes to oxidative stress in the body. A higher MAGE value indicates a higher fluctuation of glucose throughout the day or less stable glucose levels, which may be detrimental to your health. A lower MAGE value indicates a lower glucose fluctuation throughout the day or a more stable glucose, which may support your health. People with obesity have a higher MAGE than those of normal weight [9].
Studies have shown that a higher MAGE value is associated with an increased risk of death (mortality), cardiovascular events (heart attacks), diabetes, inflammation in the body, and impaired blood vessel (endothelial) function [9, 10, 11] .
5. BMI
Body mass index (BMI) is a universally used measure of body weight relative to height. It is intended to reflect the overall relative amount of body fat that a person has. BMI is calculated as a ratio of weight to height. A higher BMI ratio is generally more indicative of a higher amount of body fat. A lower BMI ratio is generally more indicative of a lower amount of body fat.
Studies have shown that an elevated BMI above the healthy weight range is associated with worse health outcomes, including higher rates of death (mortality), diabetes, heart disease, and cancer [12, 13, 14]. Being underweight is also associated with worse health outcomes [14].
Want to discover your Metabolic Healthspan?
Join Veri today.
References:
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2769652/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2699703/
- https://diabetes.org/diabetes/a1c/diagnosis
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4934381/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6709246/
- https://pubmed.ncbi.nlm.nih.gov/34624178/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6709246/
- https://link.springer.com/article/10.1007/s00592-008-0061-8
- https://pubmed.ncbi.nlm.nih.gov/24876453/
- https://www.ahajournals.org/doi/10.1161/JAHA.116.004841
- https://pubmed.ncbi.nlm.nih.gov/21854404/
- https://diabetesjournals.org/care/article/30/6/1562/30745/Effect-of-BMI-on-Lifetime-Risk-for-Diabetes-in-the
- https://www.thelancet.com/journals/landia/article/PIIS2213-8587(18)30288-2/fulltext
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5499607/

